
Despite the fact that an effective vaccine against shingles has been available for many years (since 2006) most people know someone who has had it or they have had it themselves — last year there were 120,000 new cases in Australia.
I’m very aware of the problem because it’s my peer group who are particularly vulnerable to shingles. The risk of getting it increases substantially over age 50 years, such that by age 80 years over half the population will have had at least one attack.
The burden of shingles on our community annually is substantial, not only in healthcare costs but in lost productivity. The itching, painful rash seriously interferes with the normal activities of daily living and a significant proportion of affected individuals end up with a nagging and debilitating neuralgic pain which may last months or even years (post herpetic neuralgia, or PHN).
To make things worse shingles is becoming more common globally, at least since the year 2000, for reasons that are not entirely clear.
WHY ARE WE NOT MAKING MORE INROADS ON THIS DISEASE?
So, why are we still seeing so many cases despite the availability of effective vaccination? Why aren’t more of us taking up the opportunity to be vaccinated?
• Is it because there is a lack of awareness about the condition ? That is clearly not the case as we all know someone who has had it —Newsflash! Even Justin Bieber has had it.*
*Footnote : According to a story posted on the ABC on June 11, 2022, Justin Bieber developed a rare form of shingles, known as Ramsay Hunt syndrome (herpes zoster oticus) which occurs when a shingles outbreak affects the facial nerve near one of your ears causing not only a painful shingles rash but also facial paralysis and hearing loss in the affected ear.
• Is it because people don’t know that we have the ways and means of preventing it by vaccination ? Perhaps that is a factor, in which case more publicity is required to promote greater uptake, but I don’t think this is a major reason for people not getting vaccinated.
• Is it because there has been some spillover of anti- vax sentiment into this area of public health ? Again, this may be playing a minor role but, thankfully, only a small fringe group in our society harbours these anti-scientific sentiments.
• Or is it because vaccination is only free (through the National Immunisation Program, or NIP) for those aged between 70 and 79 years of age? (Actually, the 71-79 years age group is only covered under a catch-up program that will end in Oct 2023).
The rest of us have to go through the rigamarole of seeing the GP for a prescription … then arranging for the pharmacist to order it in so that we can purchase it…then forking over $200, or more, out-of-pocket for the item…then booking in once again to see your GP to get the shot…then applying to your private health fund (if you have one) for reimbursement ( if available).
I would submit that only the most committed among us will undertake to do all this … and regardless of all the inconvenience, cost is certainly a major deterrent for some.
SO WHAT IS SHINGLES?
The term shingles is derived from the Latin cingulum, a girdle, which refers to the typical girdle-like distribution of the skin rash around the body.
Shingles, also known as herpes zoster, usually starts as a strange tingling or burning sensation, or with shooting pain and numbness in some part of the body, usually on one side of the trunk but it may be the face or ear. These sensations are often accompanied by flu- like symptoms, such as fever, headache and chills.
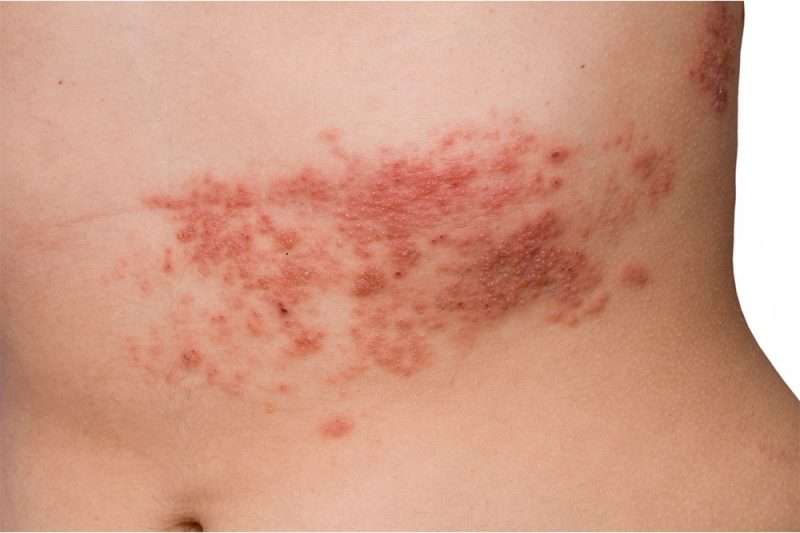
Anywhere from a day to a week after experiencing these first symptoms the tell-tale, itching, blistering skin rash appears — again, most often on one side of the trunk, but it may affect the face and even the eye or the ear, when it can potentially cause blindness, facial paralysis or hearing loss (as in Justin Bieber’s case).
Shingles can also cause –
• pneumonia
• swelling of the brain (encephalitis)
• hepatitis
• death (though rarely, from disseminated herpes zoster).
In the usual case, the blisters on the skin tend to scab over and heal after a week or two but neuralgic pain which often accompanies the rash may persist for weeks, months or even years, becoming intractable and debilitating in some.
Most patients under 30 years of age who get shingles don’t experience any persistent pain, but by age 40 years, the risk of prolonged pain lasting more than a month (PHN) increases to 33%. By age 70 years, the risk increases to 75%.
WHAT CAUSES IT?
The underlying causative agent is a virus — actually it’s the chickenpox virus, or Varicella Zoster Virus (VZV) — which first enters the body during childhood causing chickenpox *
*Footnote : Chickenpox is a cute, if not a silly name, for what can sometimes be a nasty condition which still affects millions of children in many parts of the globe. It is a strictly English language term for the virus, presumably derived from a corruption of the colloquial itching-pox.
In a bizarre evolutionary twist of self preservation, the virus remains in the body after the child recovers from a bout of chickenpox by entering the sensory nerve endings in the skin contiguous to the “pocks” or pustules. It is then transported up those nerves to reach the sensory ganglia located adjacent to the spinal cord and in the brain stem. There it finds a home in the sensory nerve ganglion cells, producing a latent infection which can remain dormant for many years.
Now and again a latent virus will reactivate, only to be shut down by our immune defences before it can multiply enough to cause perceptible damage.
If, however, immunity to the virus becomes compromised by age (so-called “immunosenescence”) or by other factors, such as immunosuppressive medications, X-ray radiation, inter current infection, cancer etc. then the next reactivation of infectious virus might enable it to multiply and travel down the sensory nerves, causing fierce inflammation of the nerve and neuralgic pain as it goes. Eventually the virus emerges around the sensory nerve endings in the skin to produce the characteristic cluster of blisters that we know as shingles.

The reason for the typical unilateral distribution of the rash is due to the fact that the pattern of sensory nerve supply to the skin is also unilateral and segmental (or “dermatomal”), as shown in the accompanying figure.
IS THERE ANY TREATMENT FOR SHINGLES?
Shingles usually clears up spontaneously in 2 to 3 weeks and seldom recurs. In most cases it doesn’t require any specific treatment, except for relief of symptoms eg. paracetamol for pain and cool, wet compresses or calamine lotion to help ease the itching and burning discomfort caused by the rash.
However, shingles which affects the upper half of the face may cause serious damage to the eye (severe conjunctivitis, keratitis and corneal ulceration) and medical attention should be sought immediately to prevent permanent impairment of sight. Treatment with antiviral drugs, such as Acyclovir, are effective in preventing eye involvement. It is imperative that treatment be started within 72 hours of the rash appearing on the face for most benefit.
CAN YOU BE INFECTED FROM A PERSON WHO HAS SHINGLES?
The good news is that you can’t contract shingles from someone with the rash.
However, if a person who has never had chickenpox or chickenpox vaccination (probably only less than 3% of the Australian population) comes into direct contact with fluid from the blisters, then they can get chickenpox. They can also pick it up from breathing in aerosols produced by coughing and sneezing by the infected person — but only if the latter has blisters in the mouth. This is because both diseases are caused by the same virus.
Consequently, people with shingles don’t need to formally isolate but they should avoid contact with –
• Pregnant women who have never had chickenpox or chickenpox vaccination (there are a number of serious health risks to the developing baby if the mother develops chickenpox in early pregnancy, including eye, brain, limb and gastrointestinal abnormalities; or if chickenpox develops during the few days before delivery, when the baby might be born with a potentially life-threatening infection called neonatal varicella.)
• Premature or low birth weight infants
• People with weakened immune systems such as people with HIV, or those receiving immunosuppressive medications or chemotherapy for cancer.
CAN YOU GET HERPES ZOSTER (SHINGLES) FROM HERPES SIMPLEX (COLD SORES)?
The terminology is a bit confusing.
Herpes zoster, (or the varicella zoster virus, VZV) which causes chickenpox and shingles, is different from the herpes simplex virus, which causes cold sores — although both belong to the same family of herpes viruses.
Both cause inflammatory clusters of blisters on the skin. In the case of herpes simplex, the blisters are usually around the lips and nostril or on the genitals, whereas zoster typically affects one or other side of the trunk in a typical dermatomal distribution.
Both share the ability to invade nerve cells once they have gained access to the body, enabling them to lie dormant for years and both can reactivate to cause recurrent outbreaks or disease – cold sores or shingles — but the two conditions are distinct and not cross-transmissible.
CAN COVID-19 VACCINATION TRIGGER SHINGLES?
VZV reactivation causing shingles may occur spontaneously or following a plethora of triggering factors, as outlined above. So it is not altogether surprising that it has been reported to occur after COVID-19 vaccination.
But is it a case of correlation or causation?
Just because an event happens around the same time as another event doesn’t imply that one causes the other.
To date, well over 11 billion doses of different COVID-19 vaccines have been administered worldwide, while there has only been a few thousand cases of associated shingles. While such cases may be underreported, their number is a far cry from the flood predicted by some authorities, early in the pandemic.
The most recent (Feb 2022) systematic review of this problem using the data base of the U.S. Adverse Event Reporting System, published an estimated incidence of approx 0.7 cases of shingles / 100,000 COVID-19 vaccinations.
The authors concluded that “the paucity of cases (almost all of a non-serious nature) makes the potential occurrence of this adverse effect negligible from a clinical viewpoint, thus supporting the good safety profile of COVID-19 vaccination, which remains strongly recommended.“
CAN SHINGLES BE PREVENTED?
There are currently two vaccines available for immunisation against shingles — Zostavax, first produced in 2006 and Shringrix, which came on the scene more recently, in 2017.
ZOSTAVAX
Is a live, attenuated vaccine formulated from the same varicella-zoster virus (VZV) as the registered varicella (chickenpox) vaccine, Varivax, which is given as a single dose.
Zostavax has a higher potency (on average at least 14X greater) than Varivax because a higher viral titre is needed to boost the immune response in adults in whom there is declining cellular immunity with age.
The overall efficacy of Zostavax vaccination against shingles in the first 3 years is 50% and against post- herpetic neuralgia (PHN) is 67%. Vaccine protection declines thereafter to about 40% after 4-7 years although it remains about 60% against PHN.
Protection against shingles is less in adults over 70 years of age compared to those in their 60s; however, there appears to be no difference in the protection offered against PHN between these two age groups.
While shingles vaccination is recommended for all adults 50 years of age and over, free Zostavax (funded by the National Immunisation Program, or NIP) is currently only available in Australia for those turning 70 years of age in a given year—and for those aged 71 — 79 years of age as part of a “catch-up” program (which will last only until Oct 2023.)
Being a live virus vaccine, it is contraindicated for use in pregnancy, because of the risk to the baby, and in people who are immunocompromised, as they are at risk of developing systemic varicella infection.
It is also not currently recommended for those individuals who have received varicella chickenpox vaccine (available since 2005 as part of the NIP for all children at 18 months of age). Fortunately, so far, it seems that the incidence of shingles in people who have had chickenpox vaccination is lower than in people who previously contracted chickenpox of the wild-type from the environment.
SHINGRIX
Instead of using a live virus, this vaccine uses a protein from the VZV virus to trigger an immune response. It is administered in 2 doses, 6 months apart.
The overall efficacy of Shingrix in preventing shingles in people in the 50-70 year age group is 97%. Vaccine efficacy is still around 91% for people older than 70 years and protection against PHN in all age groups is approximately 90%.
High vaccine efficacy has been demonstrated up to 4 years after vaccination with two doses of Shringrix and immunogenicity data suggests protection is likely to last beyond 10 years. In contrast, the effectiveness of
Zostavax significantly decreases by 5-10 years after vaccination.
The rates of local and systemic reactions are perhaps slightly higher than with Zostavax, but with both vaccines those rates are low.
Shringrix has been available in Australia from 2021 but only through private prescription; it costs $260. To date there has been no announcement about making it available for free through the NIP— even to immunocompromised individuals, who are currently not able to have Zostavax, as it contains a live virus.
The data outlined above make a strong case for NIP to switch from Zostavax to Shringrix for shingles vaccination as soon as practicable — the U.S. did so in 2020. Even the Australian Technical Advisory Group On Immunisation (ATAGI) itself stated on 26th April 2022 that “ Shringrix is preferred (my italics) over Zostavax for prevention of herpes zoster and associated complications in immunocompetent adults aged 50 years of age and over”.
I would argue that Shingrix should be made available immediately, on compassionate grounds, to those immunocompromised individuals in whom Zostavax is contraindicated.
Given that we are an enlightened, democratic first- world economy and considering the billions expended by our various governments over the past few years on universal COVID-19 vaccination, RAT tests and PCR testing clinics, it doesn’t seem unreasonable to ask that some more investment might be made into tackling the burgeoning societal scourge of shingles.
Why don’t we expand the availability of NIP-funded vaccine coverage to include most of those at risk of shingles (i.e. 60 years of age and over)?
In the meantime, if you are 50years of age, or over, and you haven’t been vaccinated, then you should consider doing so. Even if you’ve had shingles you should get vaccinated, (though you should wait until 12 months after the attack), because about 5% of people will get it again.
If you qualify for the free Zostavax vaccine, then you should avail yourself of this. However, if you don’t and if you have to pay for the vaccination out-of-pocket, then opt for Shingrix — it’s not cheap, but neither is the tab for dining out these days!
* By Dr Tony Edis MD
** In case you missed Dr Edis MD’s previous articles here they are –
#1 addressed the Intermittent Fasting trend
#2 dealt with the Food Guide Pyramid and dietary fat.
#3 discussed the ‘Lowdown’ on cholesterol and statins
#4 explained what to do when someone has a heart attack
#5 discusses the ‘miracle molecule’ Nitric Oxide
#6 asks Is too much salt in your diet bad for your health?
#7 addresses Water
PLEASE HELP US TO GROW FREMANTLE SHIPPING NEWS
FSN is a reader-supported, volunteer-assisted online magazine all about Fremantle. Thanks for helping to keep FSN keeping on!
** Don’t forget to SUBSCRIBE to receive your free copy of The Weekly Edition of the Shipping News each Friday!







